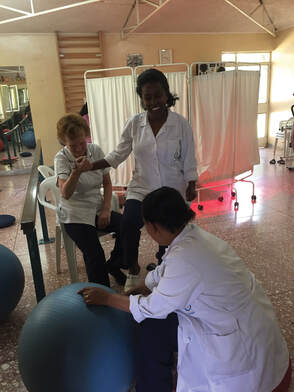
Christchurch physiotherapist Ann Johnson (expatriate of the UK), who specialises in working in gynaecology with women who experience incontinence, recently assumed the role of physiotherapy tutor to Hamlin Fistula, after her UK colleague retired from the role. In March she travelled to Addis Ababa for her first ever visit to Hamlin Fistula Hospital.

Ann writes….
“Considering I had first wanted to visit over 25 years ago it didn’t feel real when I arrived, but real it was as we were taken to the on-site guesthouse and started to review our teaching plans. Three doctors who are usually working in the outlying centres had travelled to Addis for a week’s experience in the operating theatres and physiotherapy. Between classroom and practical sessions, they would learn from us about the anatomy of the pelvic floor muscles, how to assess them when examining women and the role of the physiotherapist in strengthening the muscles which are weakened by childbirth.
Both the doctors and physiotherapists were also keen to learn more about prolapse and particularly my experience of fitting pessaries - medical devices to help support prolapses as an alternative to surgery. We discussed when they are appropriate to use as women need to be regularly reviewed medically once they are fitted; if a woman is not able to return to an out-patient clinic it could possibly cause more harm than good.
With the physiotherapists we also discussed ways to manage chronic pain and updated their exercise regime that they use for building women up whilst they await their surgery.
I had a guided tour of the hospital one morning and was really moved by meeting a lady on the ward who spoke no English or Amharic (no-one in the hospital – staff or patients - could understand her language). This meant everything that happened had to be explained by hand signals.
She was 26 years old and had 5 children. She had become urinary and faecally incontinent due to fistulas. When she arrived, she was in septic shock, very malnourished and appeared to be having psychiatric disturbances. Both her arms and legs were severely contracted, and she was very weak and unable to stand. She had had an MRI of her spine which was normal, but a CT scan of her head showed some changes to her brain. Her treatment was starting with giving her nourishing food, gentle massage to her arms and legs and exercises to get her moving again. I helped my physio colleague to sit her on the edge of the bed for the first time in, I suspect, a long time.
It is amazing to think she must have suffered like this for so long, but now she is in a good place where she will receive all the care she needs to restore her dignity and health.”